Table of Contents
Credits
Host: Sara Dong
Guests: Morgan Hui, Jonathan Darby, Max Olenski, Catriona Halliday
Writing: Morgan Hui, Max Olenski
Editing, Cover Art, Production by Sara Dong with support from the Infectious Diseases Society of America (IDSA)
Our Guests
Dr. Morgan Hui
Dr. Morgan Hui is a Basic Physician’s Trainee with an interest in infectious diseases. He is currently working as an infectious diseases registrar at Peninsula Health in Melbourne, Australia.
Dr. Jonathan Darby

Dr. Jonathan Darby is an Infectious Diseases and General Medicine Physician. He is the Head of General Medicine at St. Vincent’s Hospital Melbourne and an Associate Professor at the University of Melbourne.
Dr. Maxwell Olenski

Dr. Max Olenski is an Infectious Diseases and General Medicine Physician with an interest in tropical medicine and infections in immunocompromised hosts. He is the current Perioperative Medicine Unit Clinical Lead at Peninsula Health and a Sessional Academic with Monash University in Melbourne, Australia.
Dr. Catriona Halliday

Dr. Catriona Halliday is the Principal Hospital Scientist in charge of the Clinical Mycology Reference Laboratory at the Institute for Clinical Pathology and Medical Research (ICPMR), NSW (New South Wales) Health Pathology based at Westmead Hospital in Sydney. She is actively involved in teaching both scientific and medical staff in medical mycology and has a strong interest in culture independent tests to aid in the rapid diagnosis of invasive fungal infections and antifungal drug susceptibility surveillance.
Culture
Catriona: RBG: Of Many, One (a production about Ruth Bader Ginsburg’s life)
Max: NY Times puzzles
Morgan: golf
Jonathan: recently made baos!
Consult Notes
Case Summary
49 year old male with FSGS s/p renal transplant who presented with slow-growing painless right elbow lesion, diagnosed with mycetoma due to Falciformispora lignatilis.
Key Points
This episode discussed the possible differential diagnosis for a painless lump in a transplant recipient.
Possible causes included:
- Foregin body reaction
- Lipoma / other soft tissue neoplasms
- Lymphoma
- Infection!
- Bacterial: Skin/soft tissue infection (SSTI) such as carbuncle, syphilis, cat-scratch disease and bacillary angiomatosis, tularemia
- Fungal: disseminated aspergillosis, sporotrichosis, Rhizopus/Mucor
- Mycobacterial: TB or NTM
- Viral: cutaneous CMV, herpesvirus infections
- Parasitic: cysticercosis, trichinellosis, free-living amoebiasis, leishmaniasis
Our guests discussed some definitions and terms related to deep mycoses. Check out a summary below:
- Dematiaceous mould
- Term for a diverse group of pigmented moulds distributed worldwide (especially common in tropical and subtropical regions)
- These are dark brown / black due to presence of melanin incorporated into cellular structures
- Usually environmental saprophytes (found in soil and decaying vegetation)
- Can cause a wide range of cutaneous or disseminated infections, such as syndromes below
- Phaeohyphomycosis
- Overarching term for invasive infections caused by dematiaceous moulds (and includes non-cutaneous syndromes)
- Can occurs in both immunocompetent and immunocompromised individuals
- Chromoblastomycosis (also known as chromomycosis)
- Chronic, indolent granulomatous infection usually due to environmental inoculation of melanized moulds
- Results in chronic, progressive subcutaneous infection
- Begins at site of inoculation, affects cutaneous and subcutaneous tissues, and exhibits diverse clinical presentations
- Lesions are clinically polymorphic, the most frequent are nodular, verrucous and tumoral
- Overlying skin is often sclerosed and verrucous/wart-like
- Many different species of fungi are associated with this infection (but the three most common species are Fonsecaea, Cladophialophora and Phialophora)
- Histopathologically characterized by sclerosis
- https://dermnetnz.org/topics/chromoblastomycosis
- Mycetoma (also known as Madura foot)
- Progressive, destructive subcutaneous infection characterised by clinical syndrome of swelling/deformity (a mass) + sinus tract formation + discharge from sinus tracts with granules (grains are composed of the causative agent often embedded in cement matrix).
- Due to infection with certain fungi (eumycetoma) or certain bacteria (actinomycetoma)
- Histopathologically characterised by presence of granules. Colour & histopathological feature of the granules can help identify causative organism.
- Most common causative agent of eumycetoma = fungus Madurella mycetomatis
- Most common causative agent of actinomycetoma = bacteria Nocardia brasiliensis, Actinomadura madurae, Streptomyces saomaliensis
- https://dermnetnz.org/topics/mycetoma/

Image: Gunabooshanam, B., Johnson, T., Shalini, S. Diagnostic challenges of a spectrum of cases of Phaeohyphomycosis – A histopathological approach of rare dematiaceous (Melanized / pigmented) fungi. Jun 2020. IP Archives of Cytology and Histopathology Research. 5(2):120-125. DOI: 10.18231/j.achr.2020.025)
Catriona discussed a typical process of what happens after a sample enters the diagnostic mycology laboratory for specialized fungal cultures
- The tissue is cut into smaller pieces – not ground!
- It is important not to grind tissue samples for mycological culture because some fungi, the mucormycetes, are very fragile and grinding would destroy the hyphae and make them non viable.
- The small pieces of the tissue are pressed into the agar. Sterile tissue samples are inoculated onto Sabouraud’s dextrose agar plates enriched with brain heart infusion with and without antibiotics.
- Following inoculation, the agar plates are sealed incubated at 30C rather than 35C as fungi prefer this lower temperature for growth.
- Plates are examined for growth every few days
- If something grows, the fungus will be subcultured to a Sabouraud’s dextrose agar plate without antibiotics (while working in a biological safety cabinet). A slide culture is prepared on potato destrose agar.
- Culture based identification of fungi is primarily based on the macrosocopic appearance of the fungal colony on Sabouraud’s dextrose agar and more importantly the microscopic appearance ie the method of spore production.
- Potato dextrose agar promotes spore production of fungi better than SABs.
- If unable to assign an identification to a fungus using conventional methods, then would rely on DNA sequencing (which is now considered the gold standard for identification of fungi)
After revealing the organism, Max discussed mycetoma in more detail!
- What is mycetoma? It is a chronic, granulomatous, subcutaneous infection caused by several species of fungi and soil-inhabiting bacteria
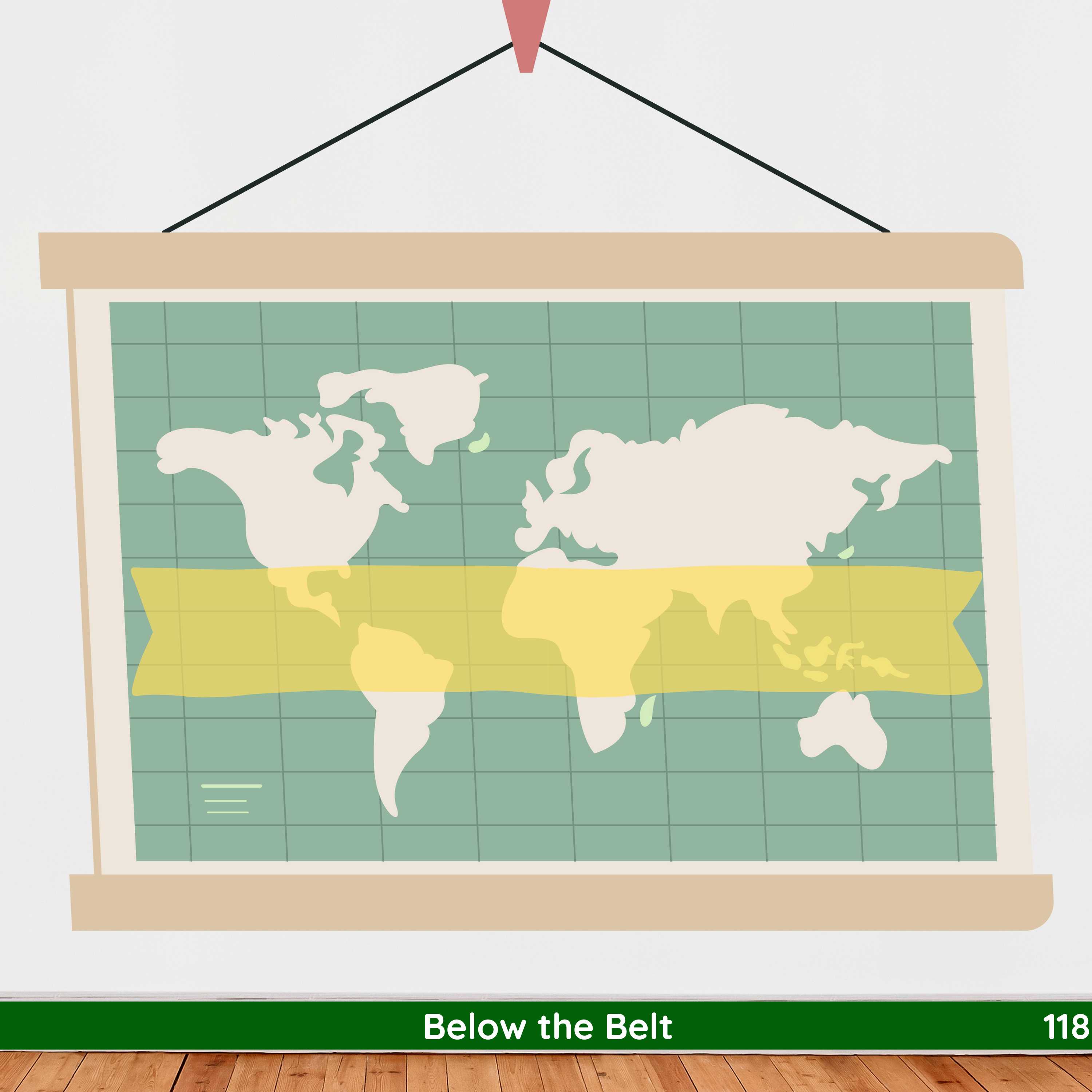
- Endemic within the so-called mycetoma belt 15°S – 30°N of the equator
- Sporadic cases reported worldwide including in temperate regions. Rare in Australia, but Higher rates in NT, Nth Qld & Indigenous population.

- Typical clinical presentation
- Triad of tumour, sinus tracts, and macroscopic grains (colonies or aggregates of the infectious organism)
- Can extend to adjacent structures including muscle, bone, lymphatics
- Risk factors: environmental/occupational exposure (’implantation mycosis’), immunocompromised state
- Mean age 33
- 3-5x more frequent amongst males
- Affected body regions: 70% feet, 10% legs, 4% arms
- Common organisms:
- Eumycetoma represent ~35% of mycetoma
- Madurella mycetomatis accounts for 75% of eumycetoma, followed by Falciforma spp and Trematospheria spp
- Differ by local epidemiology including climate, vegetation, rainfall, and soil type
- Eumycetoma represent ~35% of mycetoma
- Incubation period between inoculation and clinical manifestations is uncertain, and many patients may not recall a specific predisposing injury
- Triad of tumour, sinus tracts, and macroscopic grains (colonies or aggregates of the infectious organism)
- Atypical clinical presentation
- Can affect immunocompetent hosts. Comorbidities and immunocompromise may result in atypical / disseminated infections.
- Imported cases / link with tropics (discuss case reports)
- Often have not left country for years (>40 years since leaving Curaçao)
- Ten years prior to transplantation, he sustained a penetrating injury to his right thigh from a falling tree branch while gardening in Bermuda. The area became infected, and a 2-inch wood splinter was removed surgically, leading to complete resolution
- Atypical presentations – atraumatic foot swelling without sinus tract nor grain formation
- Diagnosis
- Clinical impression and index of suspicion are paramount. In endemic areas with limited diagnostic tools, the diagnosis is often made clinically – sometimes with that triad of tumor, sinus tracts, and discharge-containing grains.
- Presence of black grains indicates fungal etiology (eumycetoma)
- Presence of white to yellow grains may indicate fungal or bacterial infection (eumycetoma or actinomycetoma)
- Definitive diagnosis would be made by demonstration of grains and/or cavities —> fine needle aspiration to obtain material for histopathologic and cytologic evaluation
- FNA is preferred over expressed sinus material because the sinus material is more likely to be nonviable and/or contaminated
- Histopath would demonstrate hyphae, chronic granulomatous reaction with purulent center +/- presence of grain
- Grain morphology will depend on the etiology, and there are some characteristics that may be helpful for presumptive ID
- Molecular detection by PCR is possible if available. Otherwise, culture is still valuable for species identification
- Culture onto SAB
- Inoculated plates must be kept at 30 °C / 37°C for 6-8 weeks
- Imaging for determining extent
- Clinical impression and index of suspicion are paramount. In endemic areas with limited diagnostic tools, the diagnosis is often made clinically – sometimes with that triad of tumor, sinus tracts, and discharge-containing grains.
Jon discussed treatment and management
- No prospective, randomized clinical trials exist to determine the most effective drug therapy for eumycetoma – but management typically includes prolonged duration of antimicrobial agents
- In this episode’s case, selecting and monitoring therapy was a major issue owing to interactions related to calcineurin inhibitors
- For antifungal therapy:
- Consists of azole antifungal therapy based on in vitro susceptibilities
- Agents with adequate activity also include amphotericin, echinocandins, terbinafine, 5-flucytosine
- Traditional vs novel triazoles
- The earliest studies of azoles for treatment of eumycetoma were performed with ketoconazole
- Likelihood of cure favourable ≥6 months, but adverse drug reactions limit sustained therapy
- The newer triazoles, such as voriconazole and posaconazole, have the highest in vitro and in vivo efficacy, however, treatment failure has also been reported
- In countries where mycetoma is endemic, ketoconazole/itraconazole are the most commonly used with therapeutic decisions usually based on the colour of the grains
- Duration of therapy unclear but typically at least 12 months
- Surgery
- The optimal role is uncertain
- Typically if surgery is performed, will be after several months of antifungal therapy
- Limited data on surgical approach overall
- Emerging role of imaging for guidance regarding duration
Infographics
Goal
Listeners will understand the diagnosis and management of eumycetoma.
Learning Objectives
After listening to this episode, listeners will be able to:
- Compare and contrast deep mycoses terms such as phaeohyphomycosis, chromoblastomycosis, and mycetoma (eumycetoma vs actinomycetoma)
- Identify the importance of avoiding of grounding up pieces of tissue sent for fungal analysis in the microbiology lab
- Discuss the typical presentation and risk factors for eumycetoma
Disclosures
Our guests as well as Febrile podcast and hosts report no relevant financial disclosures
Citation
Olenski, M., Hui, M., Darby, J., Halliday, C., Dong, S. “#118: Below the Belt”. Febrile: A Cultured Podcast. https://player.captivate.fm/episode/d4a1486c-90a8-4918-ade6-ac5dbdb8ce89/